Hip Dysplasia (DDH) our story – keeping it in the family
When Eva was born, I was aware of Hip Dysplasia or Congenital Hip Dysplasia as it was known when I had my treatment and diagnosis, back in the 1980s. However, I wasn’t concerned about passing it on. I knew that my Dad’s cousin had had a daughter who had been in ‘froggy plaster’ as a child, just like I had, but who wasn’t as badly affected as me. I was aware it may be ‘in the family’. Still, I was shocked when, at 2 days old, Eva had her new born check and a simple ‘clunk’ during a routine manipulation changed our world.

Eva in her Van Rosen Splint
The lady doing the checks on Eva was a physio, so within what seemed like minutes, she was fitted with a little harness, not a Pavlik as in most cases, but a Van Rosen splint which does a very similar job. Things weren’t too bad with the harness. I struggled a little to breastfeed, given the new contraption and my painful caesarean scar, but I managed. Something at the back of my mind, however, told me that the 95% success rate of the harness wouldn’t apply to us.
I was finally diagnosed with hip dysplasia as a 14 month old, following months of my mum trying to convince doctors that something was not right with my legs. I underwent a closed reduction and spent a whole year in spica cast. Despite this, I soon learned to walk and all seemed normal, until I was 6 and my x rays showed that my hip was not forming properly and I would need further surgery. I had what I suspect was a Salter/ Pemberton osteotomy at the age of 7 and returned to spica, for 6 months.

My Spica
Since then, I have gone on to swim competitively, race in triathlons, get my degree and PhD, perform environmental research in difficult terrain across Africa and have two children. Which brings me back to Eva; her DDH was bilateral (in both hips) and very severe, although Graph measurements and alpha angles were still a foreign language to me then. Her right hip progressed well in harness and she wore it for nearly 6 months, by which time, her left hip was still severely dysplastic and it was obvious an operation would be needed.
She had her open reduction in 2013, followed by 5 months in spica cast with a broomstick. It was tough, my relationship had broken down and I was left as a single mother, struggling to get out of the house and unable to afford the car seat I needed to go and access help from family an hour’s drive away. At that time, the Steps grant was not enough to cover the seat and I relied on local help to get the seat and other vital supplies to keep me going. Steps were there on the phone when I needed a chat and some reassurance. Eva was sweet natured and tolerant of the cast, although putting her under anaesthetic was a horrible experience, which she fought with terrified desperation every time. I will never forget the look of betrayal in her 7 month old eyes as I held the mask over her face and watched her go ‘under’.
The time flew and she came out of cast a week before her first birthday in August. She took her first steps on Christmas Eve, a cliché, but the best gift I could have hoped for. In May 2014, her sister Islay was born. Due to our family history, she was scanned at 6 weeks despite a clear new born check. Her hip dysplasia was picked up and she spent 12 weeks in a splint before being discharged from orthopaedic care, fully fixed.
Our story would have ended there but further yearly x rays showed Eva’s hip slowly growing, but sadly, not well enough. In March 2017, she had her latest and hopefully last surgery – a Salter osteotomy at the age of 4 and 6 weeks in spica cast. It was tougher in some ways, but easier in others. I knew what to expect. I knew it would soon be over and I knew how to prepare her and explain what was going on. She literally skipped into theatre and held her own mask this time, joking about unicorns until she passed out.

Getting ready for surgery
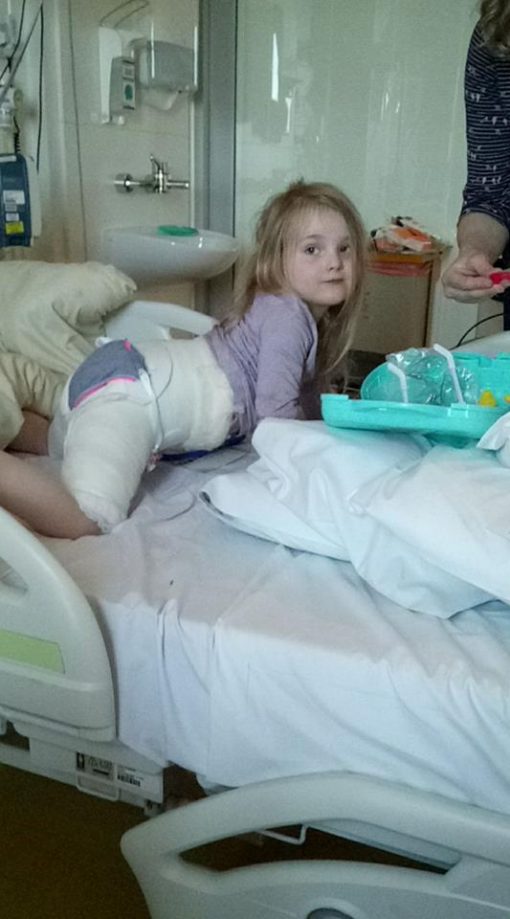
Eva Following a Salter osteotomy
Eva is out of cast now and walked as soon as it was removed. The following day, I took her to the hospital park and she climbed the climbing frame. The physios had to stop her jumping on the bed so she could have her first session. Less than a week after cast removal, she entered her school sports day; walking the races, holding her teacher’s hand and getting cheered on by her friends. The prognosis is good, her hip is well shaped and functioning. It Is unlikely she will need any more surgery, but if she does, she will cope and so will I.

Both girls, happy and healthy following DDH treatment
My hip is also bearing up well. A recent arthrogram (an MRI scan with dye in the joint to see a more accurate picture) shows a good amount of cartilage and a well rounded femoral head. I get pain, especially at night, but it is manageable. I can’t run any more, but I have learnt to row and my team are currently first in the North England Rowing Sunday league. Some people will be comforted by this story, others horrified but the research all shows that 95% of DDH cases, picked up early, can be treated successfully in a splint or harness. A few may need further surgery, but the overwhelming majority will only need a small operation and not the major surgery myself and my eldest daughter faced. We are currently participants in a research study into the genetics and inheritability of DDH and hope the study will help understanding and improve diagnosis and treatment of the condition.

My experience with Steps led me to apply for a job with the organisation and nearly 2 years later, I am still here; writing publications on familiar subjects, such as spica casts and getting your child ready for surgery and not so familiar topics, such as leg length difference, rare bone growth disorders, clubfoot and a guide for families facing amputation. I am supported by a fantastic medical board, who guide me on all my publications and by the wonderful relationship I have with NHS orthopaedic consultants, physiotherapists and many more specialist nurses and practitioners who make the high quality of the work we do possible.
